
Nurse Salina Padilla prepares an infusion of a COVID-19 antibody treatment for Dr. Prabakar Tummala at Desert Valley Hospital, Victorville, Calif., in December.
Irfan Khan/Los Angeles Times via Getty Imag
hide caption
toggle caption
Irfan Khan/Los Angeles Times via Getty Imag
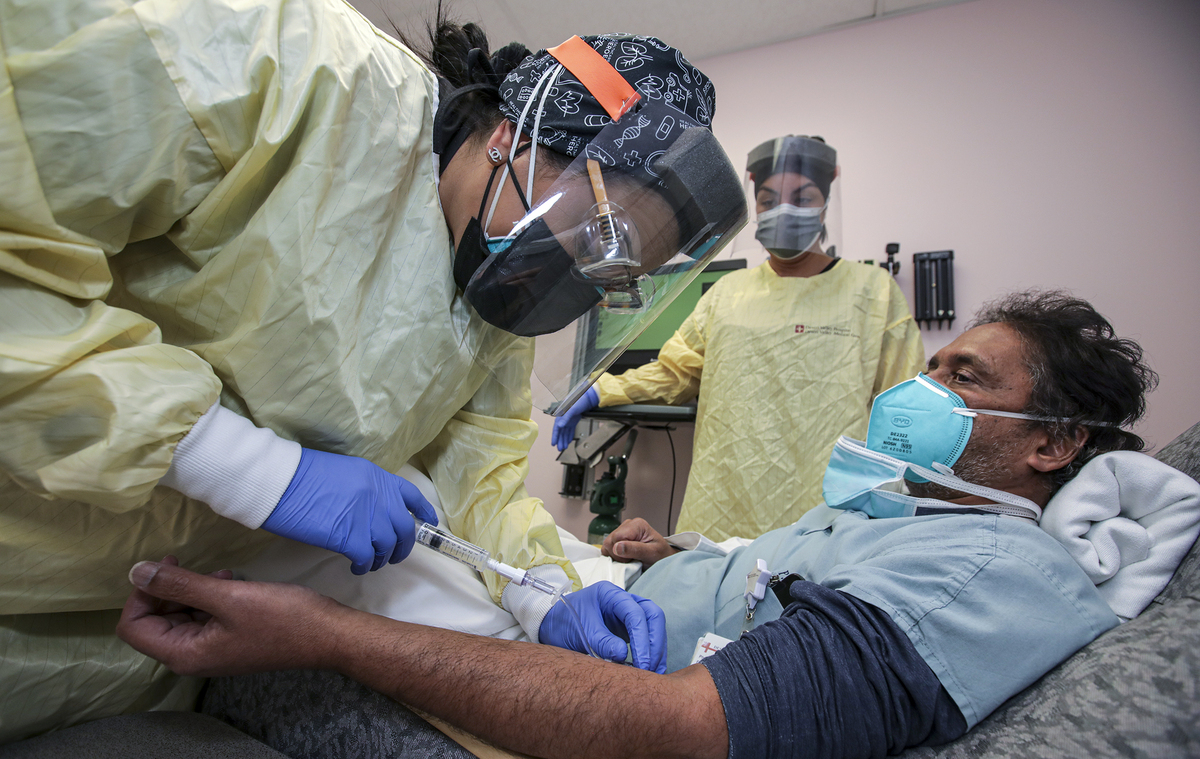
Nurse Salina Padilla prepares an infusion of a COVID-19 antibody treatment for Dr. Prabakar Tummala at Desert Valley Hospital, Victorville, Calif., in December.
Irfan Khan/Los Angeles Times via Getty Imag
Monoclonal antibody drugs are supposed to help people with mild to moderate COVID-19 avoid the hospital, but it can be a challenge to find out where the treatment is offered. NPR has heard from people across the country who have been frustrated by this.
They include Shirley Wagoner, an 80-year-old who still hits the ski slopes and helps run the family plumbing business in Spokane Valley, Wash.
First, her sons fell ill and were diagnosed with COVID-19. Then on the Monday after Christmas she came down with the symptoms of a bad cold, including a sore throat and laryngitis.
She went to her doctor’s office for a COVID-19 test and learned on New Year’s Eve that she was also sick with the disease.
Her son-in-law, Myron Lee, who lives near Chicago, had been tracking the disease closely, knew his mother-in-law would be a candidate for treatment with monoclonal antibodies.
These are drugs available nationwide through an emergency authorization. They’re designed to bind to the coronavirus to prevent it from invading cells. The government allocates the drug to states, which in turn decide how the drugs are distributed. Uptake has been irregular, in part because the medicines are cumbersome to deliver – they’re given by infusion. A committee convened by the National Institutes of Health is also not confident that the drugs actually work.
Even so, the Food and Drug Administration granted their emergency use, judging that the potential benefits outweigh the potential risks. So, Lee set about looking for somewhere in Spokane where his mother-in-law could get treated. He contacted the two companies that make the drug, Eli Lilly and Regeneron, to find it in Spokane. Information from them was discouraging.
“The weird thing is Spokane’s a pretty major city in the inland northwest,” Lee says. “It’s kind of a medical center for the whole inland northwest, but there’s not one place in Spokane that has the Eli Lilly drug.”
A representative from the Eli Lilly hotline (1-855-LillyC19) gave him phone numbers of facilities within a few hours’ drive. (Regeneron’s hotline is 1-844-734-6643).
Wagoner started calling around, including to her own doctor’s office, which falsely informed her that she would need to be hospitalized to be eligible for the drug. In fact, hospitalized patients aren’t eligible for this treatment because clinical tests indicted they were only effective early in the disease.
“Then I called the Washington State public health [department] and they’d never heard of either therapeutic,” Wagoner said.
State health officials eventually told Lee to call the big hospital in Spokane, but he simply got the runaround there and never did learn whether they provide the treatment. Wagoner finally found a clinic about an hour and a half’s drive away that would see her, but only if she could find a doctor in that town who would prescribe it.
“And then I got to thinking, by the time I had my husband drive me there, have the doctor appointment get the infusion, which takes an hour, and then they keep you two hours to make sure you don’t have a reaction, and drive home, it would almost be too much for me,” Wagoner said. “It was overwhelming.”
By then more than a week had elapsed since her first symptoms. The drugs are thought to work best within a few days of symptoms. Fortunately, she was starting to feel better on her own, so she simply gave up the search. She remembered President Trump promising that everyone could get this drug, after he himself took it.
“That was my frustration,” she said. “Trump said we could have them, but you can’t get the dang things!”
The treasure-hunt aspect for patients is slowly improving. The National Infusion Center Association built a website that now lists clinics known to offer it. (It shows that the Regeneron drug has been shipped to a clinic in Coeur d’Alene, Idaho, which is not far from Spokane).
Janelle Sabo, who manages COVID-19 drugs at Eli Lilly, says her company has fielded a couple of thousand calls asking for help locating the monoclonal antibody, and she’s happy to see that the federal government has launched a locator website, too.
As of Jan. 11, the federal website only had information for 22 states (Washington was not among them). “But hopefully that will change very soon,” Sabo says. “I know the government is as motivated as we are to make sure people know how to access this medication and to try to avoid hospitalizations.”
Because the drug has not been granted full FDA approval, Lilly is restricted in how it can promote the drug, Sabo says. It’s also a challenge that many people learn that they have COVID-19 from a testing center, not from their physician. People may in fact not have a regular physician, and doctors may not know how where to refer patients for treatment in any event.
Sabo says some COVID-19 testing sites are starting to hand out information about the antibody drugs, including information about where they are available locally. “Those are proving to be quite successful,” she says, “because very early on the patient knows what to do with their results.”
Still despite these gradual steps forward, “right now there are hundreds of thousands of doses that have been distributed and not yet used,” Alex Azar, secretary of Health and Human Services, said last week.
You can contact NPR Science Correspondent Richard Harris at rharris@npr.org.









